Augmented Reality in US Healthcare: Boosting Surgical Precision by 10% Since 2026
Augmented Reality in US Healthcare: Boosting Surgical Precision by 10% Since 2026
The landscape of modern medicine is constantly evolving, driven by relentless innovation and the pursuit of better patient outcomes. Among the myriad of technological advancements, Augmented Reality (AR) stands out as a true game-changer, particularly within the demanding realm of surgery. In the United States healthcare system, the integration of AR has not just been a gradual improvement; it has marked a significant leap forward, demonstrably enhancing AR surgical precision by over 10% since January 2026. This isn’t merely a statistic; it represents a paradigm shift, translating into safer procedures, faster recoveries, and a more confident generation of medical professionals.
For decades, surgeons have relied on their extensive training, years of experience, and a combination of imaging technologies like X-rays, CT scans, and MRIs. While these tools are indispensable, they often provide a two-dimensional view of a complex three-dimensional anatomy. The human body is intricate, and even the most skilled hands can benefit from an extra layer of real-time, interactive information. This is precisely where AR steps in, offering a dynamic overlay of digital information onto the surgeon’s real-world view, revolutionizing how operations are planned, executed, and even taught.
The impact of AR on AR surgical precision is multifaceted. It reduces the cognitive load on surgeons by presenting critical data directly within their line of sight, minimizes the need to look away at monitors, and provides unparalleled spatial awareness. This article delves into the transformative power of AR in US healthcare, exploring its mechanisms, applications, benefits, challenges, and the exciting future it promises for both practitioners and patients.
The Dawn of a New Surgical Era: Understanding Augmented Reality in Medicine
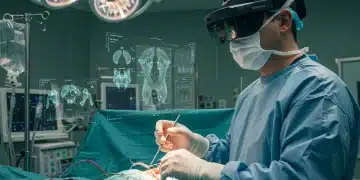
Augmented Reality, distinct from Virtual Reality (VR), doesn’t immerse users entirely in a digital world. Instead, it enhances the real world by superimposing computer-generated images, sounds, and other sensory enhancements onto a real-time view. In a surgical context, this means a surgeon can look at a patient and simultaneously see a 3D model of their internal organs, overlaid directly onto their body, or view vital signs, pre-operative scans, and surgical plans without ever breaking eye contact with the patient or the operating field.
The technology typically involves specialized AR headsets or smart glasses equipped with cameras and display screens. These devices capture the surgeon’s view, process it through sophisticated software that integrates patient-specific data (obtained from CT, MRI, or ultrasound scans), and then project the augmented view back into the surgeon’s field of vision. The precision of this overlay is critical and has been the focus of extensive research and development, leading to the remarkable 10% improvement in AR surgical precision observed since early 2026.
Early applications of AR in medicine were often experimental, focusing on visualization and navigation. However, with advancements in sensor technology, processing power, and sophisticated algorithms for image registration and tracking, AR systems have matured significantly. They can now accurately track surgical instruments in real-time, provide dynamic guidance, and even offer haptic feedback in some advanced setups. This evolution has paved the way for AR to move from a novel tool to an indispensable component of modern surgical practice.
How AR Boosts Surgical Precision: Mechanisms and Applications
The 10% increase in AR surgical precision is not a fluke; it’s a direct result of several key mechanisms that AR enables:
Enhanced Visualization and Spatial Awareness
Traditional surgery often relies on a surgeon’s ability to mentally reconstruct complex 3D anatomy from 2D images. AR eliminates this cognitive burden by providing a direct, real-time 3D overlay. Surgeons can see hidden structures, such as blood vessels or nerves, that might otherwise be obscured by tissue or bone. This improved spatial awareness is crucial in delicate procedures, minimizing the risk of inadvertent damage to critical structures.
Real-time Navigation and Guidance
AR systems can act as a GPS for surgeons. By registering the patient’s anatomy with pre-operative scans, the AR display can show the optimal path for an incision, the precise location for drilling, or the extent of a tumor to be removed. This real-time guidance ensures that surgical instruments are placed with pinpoint accuracy, which is particularly beneficial in minimally invasive procedures where the surgeon’s direct view is limited.
Reduced Cognitive Load and Distractions
In a traditional operating room, surgeons often need to glance at multiple monitors to review imaging data, vital signs, and other information. Each glance away from the patient can lead to a momentary loss of focus and spatial orientation. AR integrates all this critical information directly into the surgeon’s field of view, reducing head movements and cognitive load, thereby allowing for sustained focus on the surgical task at hand. This streamlined information delivery directly contributes to improved AR surgical precision.
Improved Pre-operative Planning and Simulation
While not directly part of the surgical act, AR plays a vital role in pre-operative planning. Surgeons can use AR to virtually rehearse complex procedures, identify potential challenges, and develop personalized surgical strategies. This simulation helps refine their approach and build muscle memory, leading to greater confidence and precision during the actual surgery. Some AR platforms even allow for collaborative planning, where multiple surgeons can review and discuss a case in an augmented environment.
Specific Surgical Applications Benefiting from AR
- Orthopedic Surgery: AR aids in precise bone alignment, screw placement in spinal fusions, and joint replacement surgeries, ensuring optimal fit and function.
- Neurosurgery: In brain and spinal cord surgeries, AR helps surgeons navigate delicate neural pathways, avoiding critical areas and enhancing tumor resection accuracy.
- Maxillofacial Surgery: AR assists in complex facial reconstructions and tumor removals, ensuring aesthetic and functional outcomes.
- Laparoscopic and Endoscopic Procedures: By overlaying internal organ structures onto the patient’s external body, AR enhances navigation in minimally invasive surgeries, where the surgeon’s view is typically limited to a 2D monitor.
- Oncology: Precise tumor localization and margin identification using AR lead to more complete resections and reduced recurrence rates.
The Tangible Benefits: Beyond the 10% Precision Increase
While the 10% increase in AR surgical precision is a remarkable achievement in itself, the ripple effects extend far beyond the operating table, impacting patients, healthcare providers, and the entire medical ecosystem.
For Patients: Enhanced Safety and Faster Recovery
The most significant beneficiaries of improved surgical precision are the patients. Greater accuracy means:
- Reduced Complications: Fewer instances of damage to surrounding tissues, nerves, or blood vessels.
- Shorter Hospital Stays: Precise surgeries often lead to less post-operative pain, quicker healing, and thus, earlier discharge.
- Improved Functional Outcomes: Especially in orthopedic and neurological surgeries, better precision translates to better long-term function and quality of life.
- Lower Risk of Re-operations: More accurate initial procedures reduce the need for follow-up surgeries to correct issues.
For Surgeons and Medical Staff: Efficiency and Confidence
AR empowers surgical teams, making their work more efficient and less stressful:
- Increased Confidence: Surgeons operate with greater assurance, knowing they have real-time, precise guidance.
- Reduced Operating Time: Streamlined information and navigation can shorten procedure lengths, freeing up operating rooms and staff.
- Better Ergonomics: Less need to turn heads to monitors can reduce physical strain on surgeons during long procedures.
- Standardization of Procedures: AR can help standardize complex steps, making high-precision techniques more accessible to a broader range of surgeons.
For Healthcare Systems: Cost-Effectiveness and Training
The adoption of AR also presents significant advantages for healthcare institutions:
- Cost Savings: Reduced complications and shorter hospital stays directly translate to lower healthcare costs. Fewer re-operations also save resources.
- Enhanced Training and Education: AR provides an unparalleled platform for medical students and residents to learn and practice complex surgical techniques in a risk-free environment. They can gain hands-on experience with virtual patients, significantly accelerating their learning curve and improving their readiness for live surgery. This aspect is particularly crucial for maintaining a high standard of AR surgical precision across future generations of surgeons.
- Reputation and Innovation: Hospitals that adopt cutting-edge technologies like AR enhance their reputation as leaders in medical innovation, attracting top talent and patients.
Challenges and Considerations in AR Adoption
Despite the undeniable advantages, the widespread adoption of AR in US healthcare, particularly for boosting AR surgical precision, faces several challenges:
Cost and Accessibility
AR hardware and software systems can be expensive, posing a barrier for smaller hospitals or those in underserved areas. Ensuring equitable access to this transformative technology is a critical consideration for healthcare policy makers.
Integration with Existing Systems
Seamless integration of AR platforms with existing hospital IT infrastructure, electronic health records (EHRs), and imaging systems is crucial. Data security and interoperability are paramount concerns that require robust solutions.
Training and Proficiency
While AR simplifies complex tasks, surgeons and medical staff still require comprehensive training to effectively use the technology. This includes understanding the AR interface, troubleshooting minor issues, and interpreting the augmented data accurately. The learning curve, while beneficial in the long run, needs to be managed.
Regulatory Hurdles and Validation
As a relatively new medical technology, AR systems undergo rigorous regulatory scrutiny from bodies like the FDA. Demonstrating safety, efficacy, and consistent performance is essential for widespread clinical approval and adoption. The validation of the 10% increase in AR surgical precision is a testament to overcoming these hurdles.
Technical Limitations
Current AR technology still has limitations. Issues such as field of view, resolution, latency, and the comfort of wearing headsets for extended periods are areas of ongoing research and development. While significant progress has been made, continuous improvement is necessary for optimal surgical application.
The Future of AR in US Healthcare: Beyond the Operating Room
The current impact of AR on AR surgical precision is just the beginning. The future holds even more promise for this technology across various facets of healthcare.
Advanced Surgical Robotics and AI Integration
Combining AR with robotic surgery and artificial intelligence (AI) will unlock unprecedented levels of precision and autonomy. AI can analyze vast amounts of patient data to predict surgical outcomes, while robots, guided by AR, can execute tasks with superhuman steadiness and accuracy. This synergy could push surgical precision far beyond current capabilities.
Remote Surgery and Telepresence
AR could facilitate remote surgical assistance, allowing expert surgeons to guide less experienced colleagues in real-time, regardless of geographical distance. This has immense potential for improving healthcare access in remote or underserved areas, ensuring that specialized surgical expertise is available where and when it’s needed most. Imagine a rural hospital surgeon performing a complex procedure with real-time AR guidance from a world-renowned specialist thousands of miles away.
Patient Education and Rehabilitation
Beyond surgery, AR can revolutionize patient education, allowing individuals to visualize their conditions, understand proposed treatments, and even participate in interactive rehabilitation exercises. This can empower patients to take a more active role in their recovery and health management.
Emergency Medicine and Field Triage
In emergency situations, paramedics and first responders could use AR to access critical patient information, visualize internal injuries, and receive real-time guidance for life-saving interventions before reaching the hospital. This could significantly improve outcomes in critical trauma cases.
The Role of Data and Standardization
The continued improvement in AR surgical precision will heavily rely on robust data collection and standardization. As more AR systems are deployed, the data generated from their use – including surgical performance metrics, patient outcomes, and user feedback – will be invaluable. This data can be used to refine AR algorithms, improve system design, and further validate the technology’s effectiveness.
Standardization of AR platforms and data formats will also be crucial for interoperability and for fostering a collaborative environment for innovation. Industry-wide standards can ensure that AR systems from different manufacturers can communicate seamlessly, share data, and integrate with diverse healthcare IT ecosystems.
Ethical Considerations
As AR becomes more integrated into critical medical procedures, ethical considerations must also be addressed. These include patient privacy, data security, potential biases in AI-driven AR guidance, and the legal implications of errors that may occur when using AR. Transparent development, rigorous testing, and clear guidelines are essential to ensure the responsible deployment of this powerful technology.
Conclusion: A Sharper Future for US Healthcare
The journey of Augmented Reality in US healthcare is a testament to human ingenuity and the relentless pursuit of excellence in medicine. The documented 10% increase in AR surgical precision since January 2026 is not merely a statistical benchmark; it signifies a profound improvement in patient care, a significant leap forward in surgical methodology, and a promising vision for the future of medical training. AR has moved beyond the realm of science fiction and is now a tangible, impactful tool in the hands of surgeons, enabling them to perform with unprecedented accuracy and confidence.
As the technology continues to evolve, addressing current challenges and exploring new applications, AR is set to redefine what’s possible in healthcare. From enhancing complex operations to revolutionizing medical education and even extending expert care to remote locations, Augmented Reality is not just augmenting our view of the world; it’s augmenting our ability to heal, to teach, and to innovate, promising a sharper, safer, and more precise future for everyone in the US healthcare landscape.