VR Healthcare Training: Reducing Surgical Errors by 30% in US Hospitals by Early 2027
The landscape of medical education and surgical training is undergoing a profound transformation, driven by the advent of cutting-edge technologies. Among these, Virtual Reality (VR) healthcare training stands out as a revolutionary force, promising to reshape how medical professionals acquire and hone their critical skills. The ambition is clear and compelling: to significantly reduce surgical errors in US hospitals, with an ambitious target of a 30% reduction by early 2027. This isn’t just a futuristic vision; it’s a tangible goal being actively pursued through innovative VR applications.
Surgical errors, while thankfully rare, can have devastating consequences for patients and profound emotional and professional impacts on healthcare providers. These errors can range from minor complications to severe, life-threatening incidents. Traditional surgical training methods, though foundational, often face limitations in providing high-volume, risk-free practice for complex procedures. Cadaver labs and live surgeries offer invaluable experience but are constrained by availability, cost, and ethical considerations. This is where VR healthcare training steps in, offering an unparalleled environment for immersive, repetitive, and safe learning.
The integration of VR into medical curricula is not merely about simulating procedures; it’s about creating an entire ecosystem of learning that fosters adaptability, critical thinking, and enhanced motor skills. By providing hyper-realistic environments, VR allows trainees to practice intricate surgical techniques, manage unexpected complications, and refine decision-making processes without any risk to actual patients. This article delves into the transformative power of VR healthcare training, exploring its mechanisms, benefits, challenges, and the roadmap to achieving that crucial 30% reduction in surgical errors.
The Imperative for Change: Addressing Surgical Errors
Surgical errors represent a critical challenge in modern healthcare. Despite rigorous training protocols and advancements in surgical techniques, human error remains an undeniable factor. Studies consistently highlight the financial and human costs associated with preventable medical errors, with surgical complications being a significant contributor. The Institute of Medicine’s landmark report, ‘To Err Is Human,’ published over two decades ago, brought this issue to the forefront, emphasizing the need for systemic changes to improve patient safety. While progress has been made, the complexity of modern surgery continues to demand innovative solutions.
Factors contributing to surgical errors are multifaceted, including lack of experience, fatigue, communication breakdowns, and insufficient exposure to rare or complex cases. Traditional training models, while effective to a degree, cannot always provide the breadth and depth of experience necessary to mitigate all these risks. Residents and fellows gain experience incrementally, often under high-pressure situations in live operating rooms. The learning curve can be steep, and the margin for error is virtually non-existent when a patient’s life is on the line.
The urgency to reduce these errors is not just about patient safety; it also has significant economic implications. Surgical complications lead to longer hospital stays, increased healthcare costs, and potential litigation. For healthcare institutions, investing in technologies that can reduce these incidents is not only an ethical imperative but also a sound financial strategy. VR healthcare training offers a proactive solution, allowing surgeons to achieve a higher level of proficiency before ever stepping into a real operating room.
How VR Healthcare Training is Revolutionizing Surgical Education
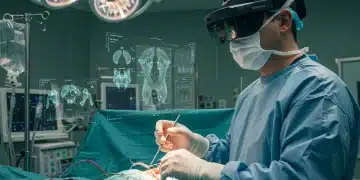
VR healthcare training leverages advanced computer graphics and haptic feedback systems to create highly realistic and interactive surgical environments. Trainees don a VR headset and are transported into a virtual operating room, where they can interact with lifelike anatomical models, surgical instruments, and even virtual patient responses. This immersive experience goes far beyond traditional video tutorials or static simulations.
Key features of VR surgical training platforms include:
- Realistic Anatomical Models: Highly detailed 3D models of organs, tissues, and skeletal structures allow for precise manipulation and understanding of complex anatomy.
- Haptic Feedback: Advanced systems provide tactile sensations, simulating the feel of cutting, suturing, and manipulating tissues, which is crucial for developing fine motor skills and dexterity.
- Procedural Step-by-Step Guidance: VR platforms can guide trainees through each step of a surgical procedure, offering immediate feedback on performance and identifying areas for improvement.
- Scenario-Based Training: Beyond routine procedures, VR can simulate rare complications, emergency situations, and various patient anatomies, preparing surgeons for a wide range of real-world challenges.
- Performance Analytics: Sophisticated software tracks every movement, decision, and outcome, providing objective data on a trainee’s performance. This allows for personalized feedback and targeted skill development.
- Multiplayer and Collaborative Modes: Some VR systems allow multiple users to train together in the same virtual environment, fostering teamwork, communication, and coordination – essential skills in any surgical team.
The ability to repeat procedures countless times without consequences is a game-changer. Trainees can experiment with different approaches, make mistakes, and learn from them in a safe, controlled environment. This iterative learning process accelerates skill acquisition and builds confidence, ultimately leading to greater proficiency and reduced errors in actual surgeries.
The Mechanism of Error Reduction: From Simulation to Skill Mastery
The pathway from VR healthcare training to a significant reduction in surgical errors is multi-faceted and relies on several key mechanisms:
1. Enhanced Skill Acquisition and Retention
VR allows for deliberate practice, a concept where individuals focus on specific areas of weakness and receive immediate feedback. This focused repetition, combined with the immersive nature of VR, leads to faster skill acquisition and better long-term retention compared to traditional methods. Surgeons can master specific movements, instrument handling, and critical decision points before performing them on patients.
2. Exposure to High-Risk and Rare Scenarios
Many surgical errors occur during unexpected complications or when encountering rare anatomical variations. VR simulations can expose trainees to these high-stakes scenarios repeatedly, allowing them to develop robust response strategies and maintain composure under pressure. This ‘pre-exposure’ significantly reduces the likelihood of panic or incorrect actions during real-life emergencies.
3. Objective Performance Measurement and Feedback
One of the most powerful aspects of VR training is its ability to provide objective, data-driven feedback. Unlike subjective evaluations in an operating room, VR systems can quantifiably measure parameters such as surgical time, instrument path efficiency, force applied, and accuracy of cuts. This data allows trainees to pinpoint specific areas for improvement and track their progress over time, fostering a culture of continuous improvement.
4. Reduced Cognitive Load in Live Surgery
When a surgeon has extensively practiced a procedure in VR, the cognitive load during a live operation is significantly reduced. They are already familiar with the steps, potential pitfalls, and instrument handling, allowing them to focus more on the patient’s unique physiological responses and any unforeseen circumstances. This reduction in cognitive load directly translates to fewer errors.
5. Team Training and Communication
Modern surgery is a team effort. VR healthcare training can extend beyond individual skill development to encompass team training. By simulating full operating room scenarios, VR can help surgical teams practice communication protocols, coordination, and crisis management, identifying and rectifying potential breakdowns before they impact patient safety. This collaborative aspect is vital for preventing errors that stem from miscommunication or uncoordinated actions.
Case Studies and Early Successes in VR Healthcare Training
While the 30% reduction target is ambitious, early adopters of VR healthcare training are already reporting promising results. Several institutions and companies are at the forefront of this revolution:
- Osso VR: This platform offers highly realistic VR surgical simulations across various specialties, including orthopedics, general surgery, and neurosurgery. Studies using Osso VR have shown that residents trained with their platform demonstrated significant improvements in surgical performance and efficiency compared to traditionally trained counterparts.
- Surgical Science: A pioneer in medical simulation, Surgical Science provides a wide range of VR and augmented reality (AR) simulators for different surgical disciplines. Their platforms are used globally to train thousands of surgeons, contributing to standardized training and improved outcomes.
- Stanford University School of Medicine: Researchers at Stanford have developed VR modules for various procedures, including cardiac catheterization and laparoscopic surgery. Their findings consistently point to VR-trained individuals performing procedures faster and with fewer errors.
- FundamentalVR: Known for its haptic-enabled VR training, FundamentalVR allows surgeons to ‘feel’ the tissue as they operate virtually. This tactile feedback is crucial for developing the nuanced motor skills required in delicate surgical procedures.
These examples illustrate a growing body of evidence supporting the efficacy of VR healthcare training. The ability to practice complex procedures repeatedly in a risk-free environment, coupled with objective performance feedback, is proving to be a powerful formula for skill mastery and error reduction.
The Roadmap to 30% Reduction: Challenges and Solutions
Achieving a 30% reduction in surgical errors by early 2027 is an ambitious goal, but one that is within reach with concerted effort. Several challenges need to be addressed:
1. Cost and Accessibility
The initial investment in VR hardware and software can be substantial for hospitals and training institutions. Solutions include developing more affordable VR systems, exploring subscription-based models for software, and securing grants or government funding for wider adoption.
2. Integration into Existing Curricula
Incorporating VR seamlessly into established medical school and residency programs requires careful planning and curriculum redesign. This involves collaboration between medical educators, VR developers, and clinical practitioners to ensure that VR training complements and enhances existing learning pathways.
3. Standardization and Validation
For VR training to be universally accepted, there needs to be standardization of training modules and rigorous validation of their effectiveness. Research studies comparing VR-trained surgeons with traditionally trained surgeons are crucial to building a strong evidence base. Accreditation bodies will play a key role in setting standards for VR-based certification.
4. Content Development and Realism
The quality and realism of VR content are paramount. Continuous development of new modules, incorporating the latest surgical techniques and anatomical variations, is essential. Collaboration between surgeons and VR developers is critical to ensure clinical accuracy and pedagogical effectiveness.
5. Instructor Training and Buy-in
Educators and supervisors need to be trained on how to effectively integrate and utilize VR in their teaching. Their buy-in is crucial for the successful adoption of VR healthcare training. Demonstrating the tangible benefits and providing adequate support will encourage widespread acceptance.
6. Data Security and Privacy
As VR platforms collect performance data, ensuring the security and privacy of this information is paramount. Robust data protection measures and compliance with healthcare regulations (like HIPAA in the US) must be a top priority for VR developers and healthcare institutions.
The Future of Surgical Training: Beyond 2027
The journey towards a 30% reduction in surgical errors by early 2027 is just the beginning. The future of VR healthcare training holds even greater promise:
- Personalized Learning Paths: AI-driven VR platforms will be able to dynamically adapt training programs to each individual’s learning style, pace, and specific areas of weakness, creating highly personalized and efficient learning paths.
- Integration with Augmented Reality (AR): The blend of VR and AR will allow surgeons to access real-time patient data, pre-operative scans, and holographic anatomical overlays during actual surgeries, enhancing precision and situational awareness.
- Remote Surgical Assistance and Tele-mentoring: VR and AR could enable experienced surgeons to remotely guide less experienced colleagues through complex procedures, effectively bridging geographical gaps and democratizing access to specialized expertise.
- Predictive Analytics for Performance: Advanced analytics could predict a surgeon’s readiness for specific procedures based on their VR training data, helping to identify potential risks and ensure optimal patient outcomes.
- Emotional Resilience Training: VR can be used to simulate high-stress surgical scenarios, helping surgeons develop emotional resilience and stress management techniques, which are crucial for maintaining peak performance under pressure.
- Patient Education and Consent: VR can also be utilized to educate patients about their upcoming procedures, allowing them to visualize the process and understand potential risks and benefits in an immersive and understandable way. This can improve informed consent and patient satisfaction.
The continuous evolution of VR technology, coupled with ongoing research and development in medical simulation, will undoubtedly lead to even more sophisticated and impactful training solutions. The goal is not just to reduce errors but to elevate the overall standard of surgical care, making complex procedures safer and more predictable for every patient.
Conclusion: A Safer Surgical Future Through VR Healthcare Training
The ambition to reduce surgical errors by 30% in US hospitals by early 2027 through VR healthcare training is a bold yet achievable objective. The evidence supporting the efficacy of immersive VR simulations is growing, demonstrating their power to enhance skill acquisition, provide safe practice environments, and offer objective performance feedback. By addressing challenges related to cost, integration, and standardization, the healthcare industry can fully harness the transformative potential of VR.
The shift towards VR healthcare training represents a paradigm change in medical education, moving from a traditional apprenticeship model to a data-driven, highly immersive, and personalized learning experience. This evolution is not just about adopting new technology; it’s about fundamentally improving patient safety, optimizing healthcare outcomes, and empowering surgeons with the confidence and precision needed to perform at their best.
As we move closer to 2027, the impact of VR healthcare training will become increasingly evident, marking a new era of surgical excellence and patient-centered care. The commitment to innovation in medical education is a commitment to a safer, more effective future for all.